PCOS (Polycystic Ovaries Syndrome): Gut Health
Polycystic Ovary Syndrome (PCOS) is a hormonal disorder causing irregular menstrual cycles, androgen excess, and potential fertility issues, often managed through lifestyle changes, medications, and, in some cases, surgical interventions.
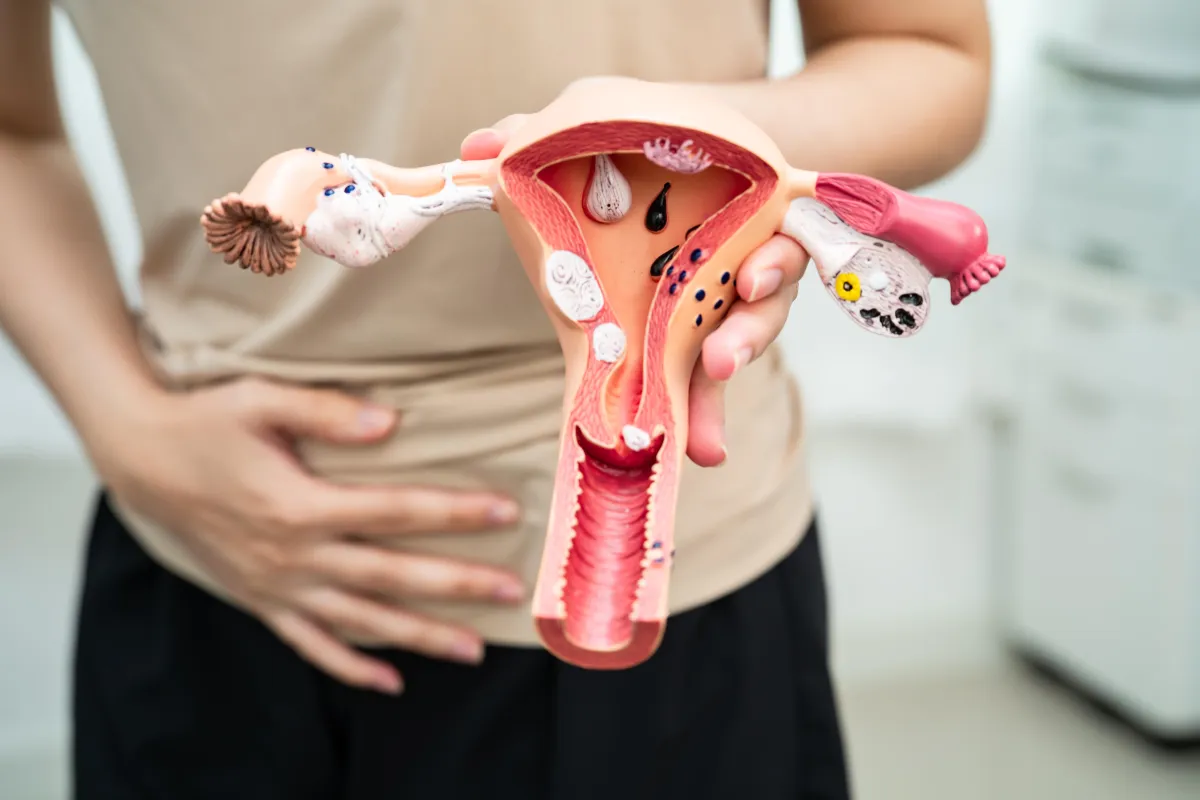
Description of PCOS (Polycystic Ovaries Syndrome):
Polycystic Ovary Syndrome (PCOS) is a prevalent hormonal disorder among women of reproductive age, characterized by a variety of symptoms due to elevated levels of male hormones (androgens). Key symptoms include irregular menstrual cycles, excess facial and body hair (hirsutism), severe acne, and in some cases, male-pattern baldness. Additionally, polycystic ovaries, which are enlarged and contain multiple small cysts, may be present, although not all women with PCOS exhibit these cysts.
The causes of PCOS are complex and not entirely understood, but genetic factors play a significant role. Many women with PCOS also have insulin resistance, which can lead to higher insulin levels that further boost androgen production by the ovaries. Hormonal imbalances and inflammation are also believed to contribute to the development and progression of PCOS. Managing PCOS often involves lifestyle modification, such as diet and exercise, which can improve symptoms and promote regular ovulation.
Medications are also commonly used, including birth control pills to regulate menstrual cycles, metformin to enhance insulin sensitivity, and anti-androgens to reduce excess hair growth and acne. For those seeking to become pregnant, medications like clomiphene may be used to stimulate ovulation. In certain cases, surgical interventions, such as ovarian drilling, can be considered to induce ovulation. Women experiencing symptoms suggestive of PCOS should seek medical advice to receive an accurate diagnosis and determine the most suitable treatment strategy tailored to their individual health needs.
Role of Gut Imbalances in Polycystic Ovaries Syndrome:
Polycystic Ovarian Syndrome (PCOS) is a common endocrine disorder that affects women of reproductive age, characterized by symptoms such as irregular menstrual cycles, excessive androgen levels, and polycystic ovaries. Emerging research suggests a connection between gut health and PCOS, indicating that gut imbalances might play a role in the condition.
Introduction: PCOS is primarily considered a hormonal disorder, but recent findings suggest a potential link between gut microbiota imbalances and PCOS. The gut microbiome, consisting of trillions of microorganisms, plays a crucial role in modulating various bodily functions, including metabolism and immune responses.
Gut Imbalances and Their Influence on PCOS: The theory posits that dysbiosis, an imbalance in gut microbiota, can exacerbate or potentially contribute to the development of PCOS. Gut dysbiosis may affect the metabolic and hormonal pathways relevant to PCOS by influencing insulin resistance, inflammation, and androgen levels. Insulin resistance is a common feature of PCOS, and gut imbalances can exacerbate this by affecting glucose metabolism and insulin signaling pathways.
Scientific Findings: Research has highlighted that women with PCOS often exhibit altered gut microbiome compositions compared to those without the condition. Studies suggest that microbial metabolites, such as short-chain fatty acids (SCFAs), which are products of dietary fiber fermentation, play a role in inflammatory and metabolic regulation. A decrease in beneficial SCFA-producing bacteria in the gut may lead to increased inflammation and insulin resistance, both of which are significant factors in PCOS pathology.
Potential Interventions: Restoring a healthy gut microbiome may help manage PCOS symptoms. Probiotics, prebiotics, and dietary modifications aimed at increasing fiber intake and reducing processed foods may support healthy microbiota composition. Such interventions could help reduce insulin resistance and inflammation, potentially alleviating some symptoms of PCOS.
Conclusion: While more research is needed to fully understand the extent of the relationship between gut imbalances and PCOS, current evidence suggests that maintaining a balanced gut microbiota could be beneficial for managing PCOS. Continual findings in this area underline the importance of considering gut health in the holistic management of PCOS.
